Think back to what you were like ten, fifteen years ago. A different hairstyle, perhaps an unfortunate pair of striped pants? We all change, for better or for worse. Just as you undergo changes in your lifetime, so too have CPR practices evolved over the years. This article will prevent you from ever practicing an outdated form of CPR (embarrassing) and keep you informed as to the context and reasoning behind CPR’s progression.
Since the development of cardiopulmonary resuscitation in 1960, the American Heart Association (AHA) and International Liaison Committee on Resuscitation (ILCOR) have worked together to analyze previous years’ CPR guidelines. The two work to release new CPR protocols every five years and ensure that CPR is more comfortable to perform and more efficient for the layman.
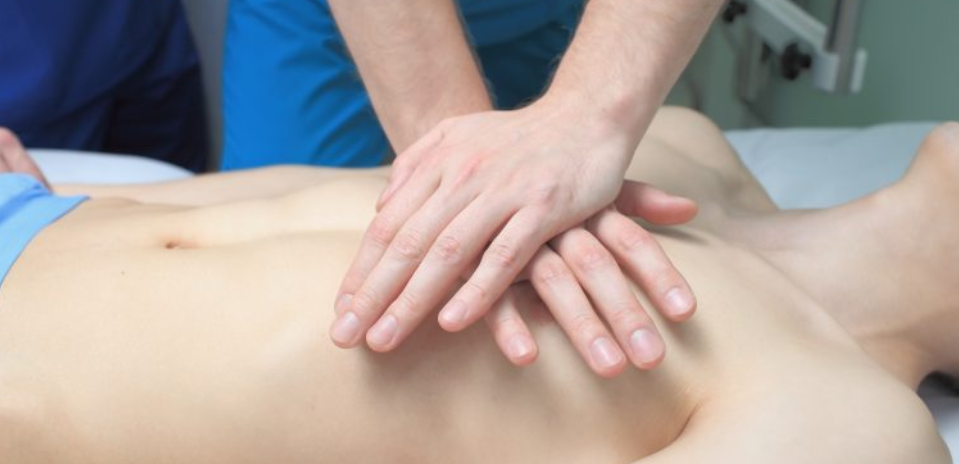
Emphasis on Chest Compressions
One of the more widespread changes to CPR guidelines was the emphasis on chest compression. The American Health Association has increased the focus of hands-on CPR or compression-only CPR for people who are not CPR-trained but find themselves in a scenario that calls for it.
In addition, there have been changes to how those aforementioned compressions should be performed. The recommended rate of chest compressions increased from the initial rate of 60 compressions per minute to around 100 compressions in the first 50 years following the creation of the AHA. Further research and development readjusted that rate to the current recommendation of 115-120 compressions per minute. Why has the consensus settled around that range? The likelihood of resuscitation is at its peak when the chest compressions land in that range, but begin to decline once compressions rise over 125 per minute.
When it comes to executing the compressions, best practices have also evolved. Using the weight of the upper body to perform compressions should only be utilized to press down on the chest. Relieve the weight while waiting for the chest to recoil. A since-dismissed practice known as “compression-decompression resuscitation,” is where the abdomen is pressed down on to ensure that the chest recoils. This method has since gone medically obsolete.
AED Guidelines
Automated external defibrillators, commonly known as AEDs, were widely introduced in 1995 (although developed decades earlier) to determine if ventricular fibrillation (VF) -a process where the heart beats in a rapid and erratic pattern– was occurring in a patient. Later guidelines limited AED usage to chest compressions where three shocks were administered before beginning the compressions. Research at the time highlighted that this would be a useful measure to make chest compressions more efficient, but that was found to be ineffective. Later standards advised rescuers to instead give compression before using the AED if an AED was not within reach. Individuals giving CPR are now advised to continue compressions right after administering a shock.
Compressing Deeply
When you compress, you really want to compress. Not enough to crush the chest, but enough that you can see the chest sinking as you press. In the past, the recommended depth of compressions was between 1.5 to 2 inches, but now, an acceptable deepness is at least 2 inches, but no more than 2.5. It can be uncomfortable or seem like you’re damaging the patient to push that hard, and you’re not entirely wrong. However, saving a life is more important than the potential for a few broken ribs. Things can always go wrong in CPR, but that doesn’t absolve a bystander of the obligation to step in if they are capable.
Providing Care Immediately
Previous guidelines suggested calling 911 before performing CPR. However, new directions direct providing care for a few minutes before calling an emergency number. This action ensures that blood flow is sustained in the body for the first few minutes, which are the most important. It’s a commonly stated figure, but when CPR is immediately performed, it can double or triple the rate of survival.
Change in Order
Original CPR methods emphasized the ABC method, standing for airway, breathing, and compressions. In 1995, the AHA recommended adding a D (for defibrillation) to the standard, so it read ABCD’s of CPR. First, you would clear the person’s airway, then provide rescue breaths, before delivering compressions and defibrillating. However, in 2010, the AHA changed the guidelines, so the order read CAB. Compressions were emphasized first because they help sustain the blood flow to the brain. Providing chest compressions minutes later, like the old guidelines suggested, meant that crucial time to save an individual’s life was being wasted away. The CAB order supports first providing compressions, before cleaning out the airway and then giving rescue breaths.
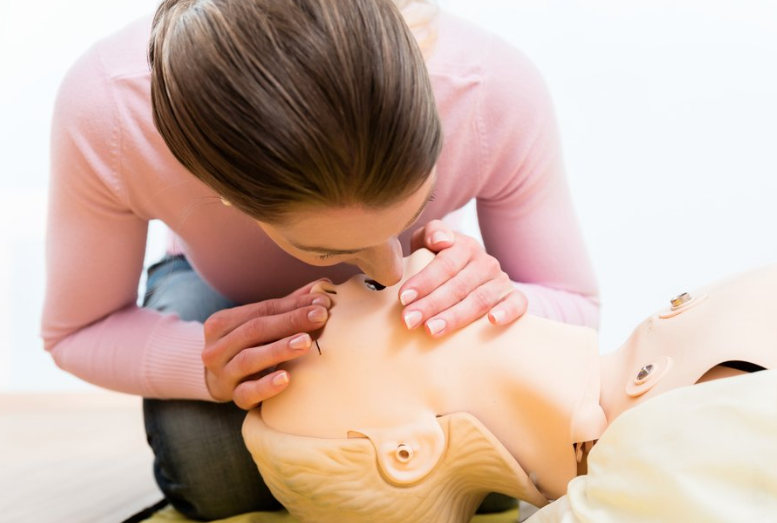
Rescue Breaths Are Not Emphasized
With the emphasis on chest compressions, rescue breaths may appear mostly useless. However, that is not the case. Rescue breaths are incredibly important, but the American Heart Association no longer actively recommends administering these because the steps can be complicated to remember in times of stress. Studies have shown that people not medically trained easily remember CPR if the steps are simple. In addition, individuals providing CPR do not have to worry about exposing themselves to diseases or giving incorrect breaths and can go straight to chest compressions, which raises a patient’s survival rate the most. Other research has shown that bystanders are less willing to perform CPR when they contemplate doing rescue breaths. So removing rescue breaths as a necessity makes bystanders more willing to help victims on the scene.
Checking for Life
The most recent recommendations on this topic say to avoid checking for a pulse until a few cycles of CPR and (maybe) rescue breaths are completed. This change helps reduce the time it takes to resume compressions, which are again crucial to victim survival. Previous best practices were to check pulses quickly and then look for signs of circulation such as discoloration of the lips, face, or extremities before performing CPR. However, these techniques wasted valuable time, which the AHA has emphasized could be better used on compressions.
Compressions to Rescue Breaths Ratio
Ten years ago, the recommended rate was 15:2 or one breath per fifteen compressions with two-person CPR. However, that rate has changed to 30:2. This change highlights the overarching shift to emphasizing chest compressions above all else. Now, chest compressions are considered the most important part of CPR, while a decade ago, it was breathing. The American Heart Association believes it is better to circulate blood that is not fully oxygenated (no rescue breaths) than to oxygenate the blood but not create enough blood flow (fewer compressions) for the blood to flow back to the brain.
As survival depends on the quality of basic life support before getting to the hospital, it is essential to have practices that increase the effectiveness of CPR procedures. Over the last 50 years there have been substantial changes that have achieved just that, and now the future remains full of even more possibilities.





